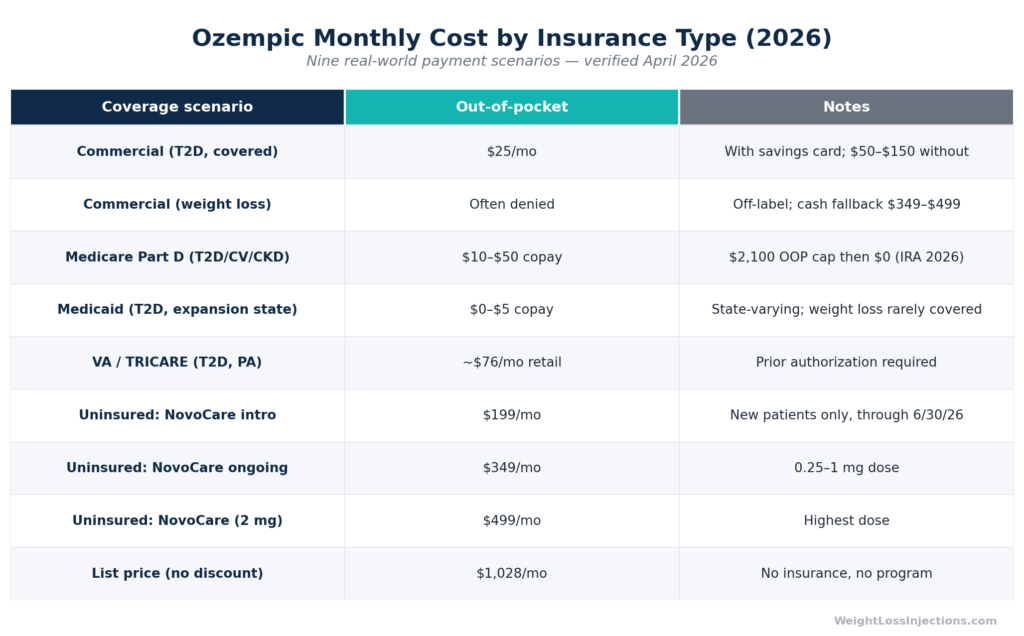
Ozempic Cost by Insurance Type 2026
Ozempic list price is $1,028/mo. With commercial insurance covering the T2D indication plus the Novo Nordisk savings card, that drops to $25/mo. Medicare Part D covers Ozempic for diabetes, cardiovascular risk, and chronic kidney disease at $10–$50/mo copay, with a $2,100 annual out-of-pocket cap after which covered drugs cost $0, but the savings card does not apply to Medicare.
For uninsured patients, NovoCare self-pay starts at $199/mo introductory (through June 30, 2026) and $349–$499/mo ongoing. Weight loss coverage, whether commercial, Medicare, or Medicaid, is a different and harder story.
How Ozempic Is Priced in 2026
Ozempic (semaglutide injection) carries a wholesale acquisition cost of $1,028/mo, the manufacturer’s list price before any insurance negotiation, rebate, or savings program. That number is the starting point for every cost calculation, but it is not what the vast majority of patients pay.
Three variables determine your actual out-of-pocket cost: (1) your insurance type, (2) the clinical indication on your prescription, and (3) which savings or assistance programs you qualify for. Because Ozempic is FDA-approved for type 2 diabetes (T2D), cardiovascular risk reduction, and chronic kidney disease (CKD), but not for weight loss, each payer handles coverage for those distinct uses very differently. Weight loss is off-label, and that label distinction is the single biggest driver of insurance denials.
This guide breaks down what each major payer pays, where the friction points are, and what your options are when insurance doesn’t cooperate.
Ozempic List Price vs. Insured Costs: Summary Table
The table below uses verified pricing as of April 2026. Copay ranges reflect plan-to-plan variation before any savings programs are applied.
| Scenario | Monthly Cost |
|---|---|
| List price (no discount, no insurance) | $1,028 |
| Commercial insurance, T2D covered + savings card | $25 |
| Commercial insurance, T2D covered, no savings card | $50–$150 copay |
| Commercial insurance, weight loss off-label | Often denied; cash fallback $349–$499 |
| Medicare Part D, T2D/CV/CKD indication | $10–$50 copay; $2,100 annual OOP cap |
| Medicaid, T2D indication (expansion state) | $0–$5 copay |
| VA/TRICARE, T2D with PA | ~$76/mo retail |
| NovoCare self-pay, new patient intro | $199 (through June 30, 2026) |
| NovoCare self-pay, ongoing 0.25–1 mg | $349 |
| NovoCare self-pay, 2 mg | $499 |
Sources: Ozempic.com savings card page; GoodRx Ozempic; GoodRx Medicare Part D OOP cap 2026; SingleCare TRICARE Ozempic coverage
Formulary tier placement is a key variable. Most commercial plans classify Ozempic as Tier 3 (preferred brand) or Tier 4 (specialty), which directly governs the copay range before the savings card reduces it to $25.
Commercial and Private Insurance
Coverage for Type 2 Diabetes
Commercial insurance is the most favorable environment for Ozempic access. When a plan’s formulary includes Ozempic for the T2D indication, most commercial plans cover it, though prior authorization is nearly universal, and step therapy (typically a requirement to have tried metformin first) is common in roughly half of commercial plans.
With coverage active and the Novo Nordisk savings card enrolled, eligible commercially insured patients pay as little as $25/mo for any dose, with maximum savings of $100/month for up to 48 months (or $200/$300 for 2- and 3-month supplies). Without the savings card, specialty-tier copays commonly land in the $50–$150/mo range depending on plan structure and deductible phase.
To activate the $25 rate:
- Confirm Ozempic is on your plan’s formulary for T2D.
- Enroll in the Novo Nordisk savings card at Ozempic.com — government beneficiaries (Medicare, Medicaid, TRICARE, VA) are excluded.
- Present the card at your pharmacy; it processes outside your insurance separately.
WeightLossInjections.com editorial note: The savings card is only valuable once your plan has confirmed coverage for Ozempic. If your plan puts Ozempic on a non-covered tier, the card cannot be stacked on top of a denial, it functions as a copay reducer, not a full price program. Call your plan’s pharmacy line and confirm formulary placement and PA status before banking on the $25 rate.
Commercial Coverage for Weight Loss
Ozempic is not FDA-approved for weight loss. That legal reality means that when a prescriber’s claim codes are obesity-only, most commercial payers will deny it. The labeled weight-loss alternatives, Wegovy (semaglutide, higher dose) and Zepbound (tirzepatide), have better insurance prospects for obesity indications, though prior authorization and step therapy remain nearly universal.
If your prescriber believes Ozempic is appropriate for weight management and you have a T2D co-diagnosis, the T2D indication may carry the claim. In purely weight-loss-only scenarios, expect a denial and a PA fight. The savings card is still available to commercially insured patients who use Ozempic off-label, as long as the plan has any coverage for the drug — but a plan that declines the claim entirely renders the card moot.
Medicare Part D in 2026
What Medicare Covers
Medicare Part D covers Ozempic for its three FDA-approved indications: T2D glycemic control, cardiovascular risk reduction in T2D patients with established CV disease, and CKD risk reduction in T2D patients with chronic kidney disease (the FLOW trial indication, approved January 28, 2025). Federal law, the Medicare Prescription Drug, Improvement, and Modernization Act (MMA), prohibits Part D from covering drugs prescribed solely for weight loss, so Medicare does not cover Ozempic for weight management.
Most Part D and Medicare Advantage plans place Ozempic on Tier 3 or Tier 4 specialty. During the initial coverage phase, beneficiaries typically pay 25% coinsurance, which on a $1,028 list price translates to roughly $230–$260/mo until the annual OOP cap is hit.
The $2,100 Out-of-Pocket Cap
The most significant 2026 Medicare change for high-cost drug users is the Inflation Reduction Act’s annual out-of-pocket cap: $2,100 per year. After a beneficiary’s total Part D out-of-pocket spending (including deductibles and copays) reaches $2,100, the plan covers 100% of covered drug costs for the rest of the calendar year.
For Ozempic users who enter the year in the deductible phase, the Part D deductible in 2026 is capped at $615. CMS confirmed the $2,100 OOP threshold in its final 2026 Part D redesign instructions. Practically, a Medicare beneficiary paying ~25% coinsurance on a $1,028 drug can reach the $2,100 cap within 3–4 months, after which Ozempic costs $0 for the remainder of the year. According to JAMA Health Forum analysis, beneficiaries on a single high-cost specialty drug often reach the catastrophic phase between March and April.
CMS also introduced an optional Medicare Prescription Payment Plan (MPPP) in 2025 that allows spreading out-of-pocket costs across the year in monthly installments, reducing the sticker shock of early-year fills.
The Savings Card Does Not Apply to Medicare
This is the most common point of confusion. The Novo Nordisk savings card explicitly excludes government beneficiaries. Medicare patients cannot use the $25 savings card. The NovoCare patient assistance program (PAP), which provides Ozempic at no cost to uninsured low-income patients, similarly no longer covers Medicare Part D patients, because most Medicare Part D plans now cover Ozempic. Instead, Medicare beneficiaries with limited income should look at the Part D Extra Help / Low Income Subsidy (LIS) program, which can reduce out-of-pocket drug costs substantially.
Weight Loss Under Medicare: BALANCE Model Bridge (July 2026)
For beneficiaries who want GLP-1s specifically for weight management, CMS announced the BALANCE Model (Better Approaches to Lifestyle and Nutrition for Comprehensive Health) in December 2025. A six-month “bridge” program is scheduled to launch July 2026, allowing qualifying Medicare beneficiaries to access GLP-1 weight-loss medications at a $50/mo copay. This bridge operates outside of standard Part D coverage and applies to labeled weight-management products (Wegovy, Zepbound), not to Ozempic for off-label weight loss. Full Part D integration is expected in January 2027 for participating plans.
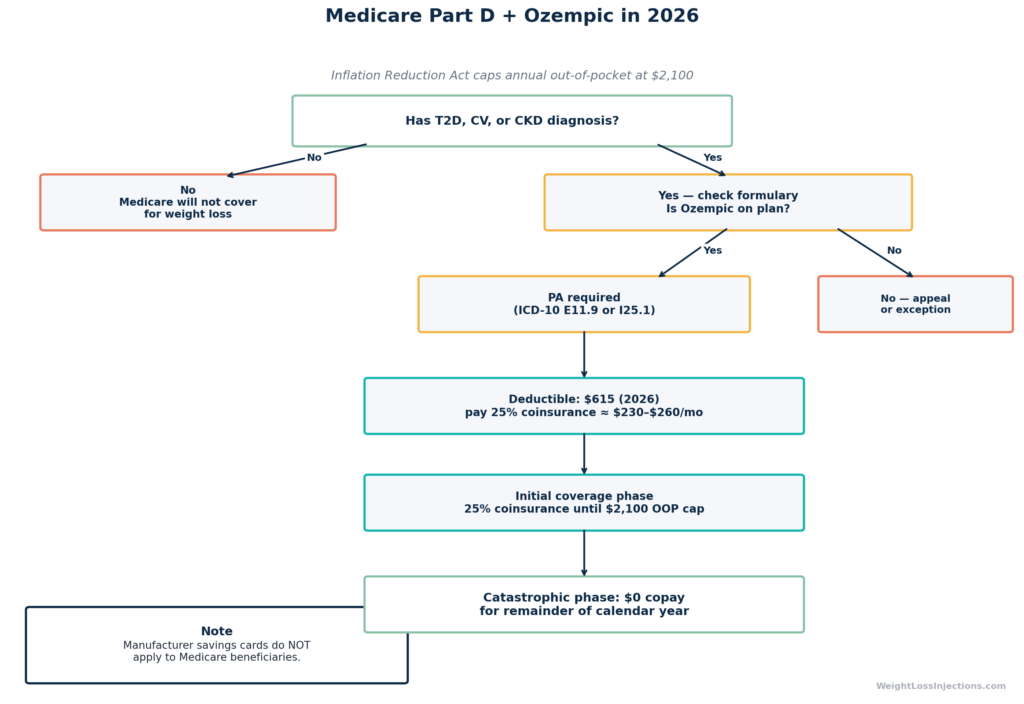
Medicare Part D Ozempic Cost Flow 2026
Medicaid Coverage
T2D Indication: Usually Covered, With PA
Medicaid’s approach to Ozempic is mostly positive for the T2D indication but heavily gatekept. According to GoodRx data, nearly all Medicaid enrollees have some coverage for Ozempic when used for FDA-approved conditions, but close to three in four face a prior authorization requirement, and more than half are subject to step therapy. The typical step-therapy requirement means documenting an adequate trial of metformin (usually 60 days or more) or a contraindication to it before Ozempic is approved.
When approved, Medicaid copays for Ozempic are low, typically $0–$5/mo for most enrollees.
Weight Loss: Almost Never Covered
Federal law does not require states to cover weight-loss drugs, and most states take the opt-out. As of early 2026, only 13 state Medicaid programs cover GLP-1s for obesity treatment: Delaware, Kansas, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, North Carolina, Rhode Island, Tennessee, Utah, Virginia, and Wisconsin. Pennsylvania eliminated GLP-1 weight-loss coverage effective January 1, 2026, and the trend toward restriction is accelerating in 2026 as states face budget pressure.
Medicaid patients cannot use the Novo Nordisk savings card or the NovoCare PAP. Government insurance enrollment disqualifies a patient from both programs.
Checking Your State’s Coverage
The fastest approach is searching “[Your State] Medicaid preferred drug list Ozempic”, every state publishes its PDL through the state health department or Medicaid agency website. If Ozempic is listed as nonpreferred, prior authorization requirements increase; if it’s not listed at all for a given indication, your prescriber can request a formulary exception.
VA and TRICARE Coverage
TRICARE
TRICARE covers Ozempic for type 2 diabetes under plans including TRICARE Prime, TRICARE Select, and most premium-based plans. Prior authorization is universally required; for military pharmacy fills, a medical necessity form is also required as of August 31, 2025, per Defense Health Agency guidance. Ozempic is a non-preferred agent on TRICARE’s formulary (Trulicity, dulaglutide, is the preferred GLP-1 for T2D), so prescribers must justify Ozempic over the preferred alternative.
TRICARE retail pharmacy copay for a 30-day supply of Ozempic is typically $76 for non-active duty beneficiaries. Fills at military treatment facility pharmacies may carry a lower copay or be $0 for active duty, subject to formulary approval, according to SingleCare’s TRICARE analysis. TRICARE does not cover Ozempic for weight loss without a T2D diagnosis.
VA
VA coverage follows a national formulary structure, with Ozempic available for T2D with prior authorization. Veterans seeking Ozempic for weight management only, without a T2D diagnosis, face the same off-label barrier as other federal payers. PA requirements and preferred-agent substitution rules apply. Contact your VA primary care team or the VA Pharmacy directly to confirm current formulary tier and PA requirements.
How to Check Your Coverage and Get Approved
If you have insurance that may cover Ozempic, a four-step process maximizes your chances:
Step 1: Look up your formulary. Log into your plan’s member portal, search “Ozempic” or “semaglutide,” and note the tier level and any coverage restrictions listed.
Step 2: Confirm the indication on your claim. Prior authorization forms typically require an ICD-10 code, E11.9 (type 2 diabetes without complications) or I25.10 (atherosclerotic heart disease) are the most commonly approved pathways. Your prescriber’s office submits this; ensure the diagnosis on file matches the indication.
Step 3: Submit prior authorization with documentation. Your prescriber will need to provide HbA1c levels, list of previously tried diabetes medications, and clinical justification. For step therapy, documentation of metformin trial or contraindication is central.
Step 4: If denied, appeal. A formal internal appeal letter, followed by an external review if needed, resolves a meaningful share of denials, particularly when a prescriber can document medical necessity clearly. A basic appeal letter outline should include:
- Patient name, date of birth, insurance member ID, Rx claim number
- Specific denial reason cited by the plan
- Clinical rationale from the prescriber: diagnosis, A1C value, prior therapies tried, clinical outcome goals
- Reference to FDA-approved indication language from the Ozempic prescribing information
- Request for expedited review if medically urgent (e.g., uncontrolled A1C, recent CV event)
Savings If Denied or Uninsured: NovoCare, GoodRx, PAP
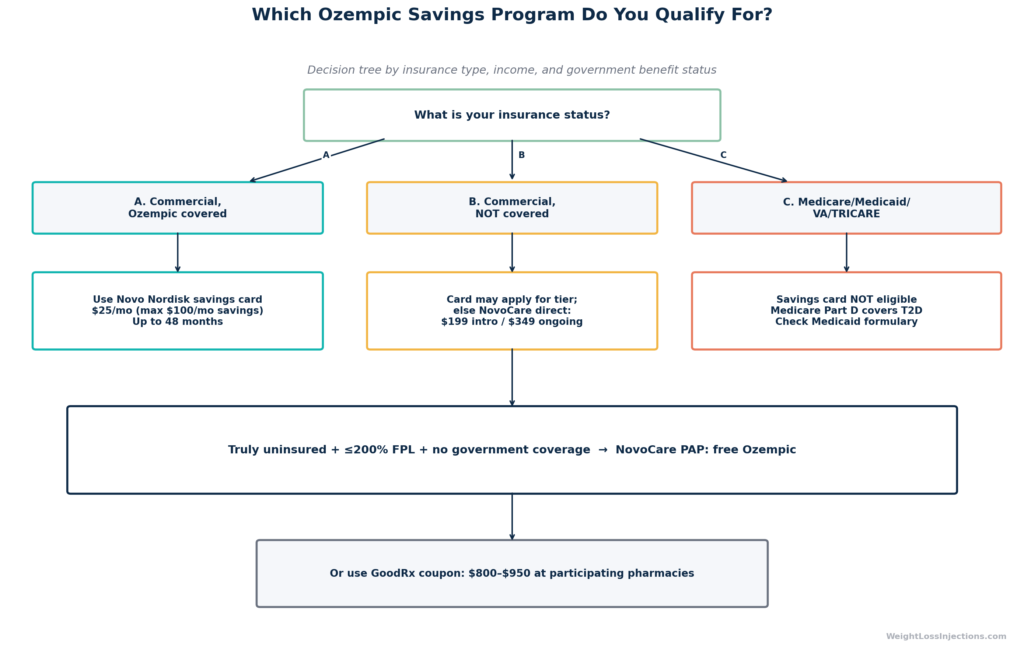
Ozempic Savings Eligibility Decision Tree
NovoCare Self-Pay Program (Uninsured / Self-Pay)
For patients without commercial insurance, or those whose commercial plan does not cover Ozempic , Novo Nordisk offers direct pricing through the NovoCare Pharmacy, per Ozempic.com’s savings page:
| Patient Type | Dose | Monthly Cost |
|---|---|---|
| New patient (intro offer through 6/30/2026) | 0.25 mg or 0.5 mg | $199 |
| Ongoing (after first 2 fills) | 0.25 mg, 0.5 mg, or 1 mg | $349 |
| Ongoing | 2 mg | $499 |
These prices are processed outside of insurance, do not count toward deductibles or OOP maximums, and require a valid Ozempic prescription. Government beneficiaries, Medicare, Medicaid, TRICARE, VA, are excluded from NovoCare self-pay pricing.
GoodRx Coupons
GoodRx reports coupon prices that closely parallel NovoCare pricing, as of April 2026:
- 0.25/0.5 mg pen (2 mg/3 mL): ~$199 with GoodRx coupon
- 1 mg pen (4 mg/3 mL): ~$349
- 2 mg pen (8 mg/3 mL): ~$499
GoodRx coupons cannot be combined with insurance, they are used in lieu of insurance. Government beneficiaries can generally use GoodRx discounts as long as they are not billing a federal program for the same fill.
Patient Assistance Program (PAP): Free Ozempic for Low-Income Uninsured
Novo Nordisk’s NovoCare PAP provides Ozempic at no cost to patients who qualify, per NovoCare PAP program details:
- Income limit: total household income at or below 200% of the federal poverty level (FPL) for Ozempic specifically (the FPL threshold is stricter for Ozempic than for other Novo Nordisk products, which allow up to 400% FPL)
- Insurance status: no commercial insurance; no Medicaid; no VA benefits; Medicare patients are excluded from Ozempic PAP because most Medicare Part D plans now cover the drug
- U.S. citizen or legal resident; valid Ozempic prescription required
The 200% FPL income limit for Ozempic is an important detail that many sources get wrong, Novo Nordisk explicitly states this in the 2026 PAP terms. For a single-person household in 2026, 200% FPL is approximately $30,120 annually.
Our take at WeightLossInjections.com: The NovoCare PAP is genuinely valuable for uninsured patients who meet the income test, but the 200% FPL cutoff leaves out a large share of the uninsured middle-income population. If you earn above that threshold and are uninsured, the $199 introductory NovoCare self-pay offer is the most cost-efficient entry point, but only through June 30, 2026. After that, the ongoing $349/mo rate for 1 mg is what most self-pay patients budget for.
GLP-1 Cost Comparison: Ozempic vs. Alternatives
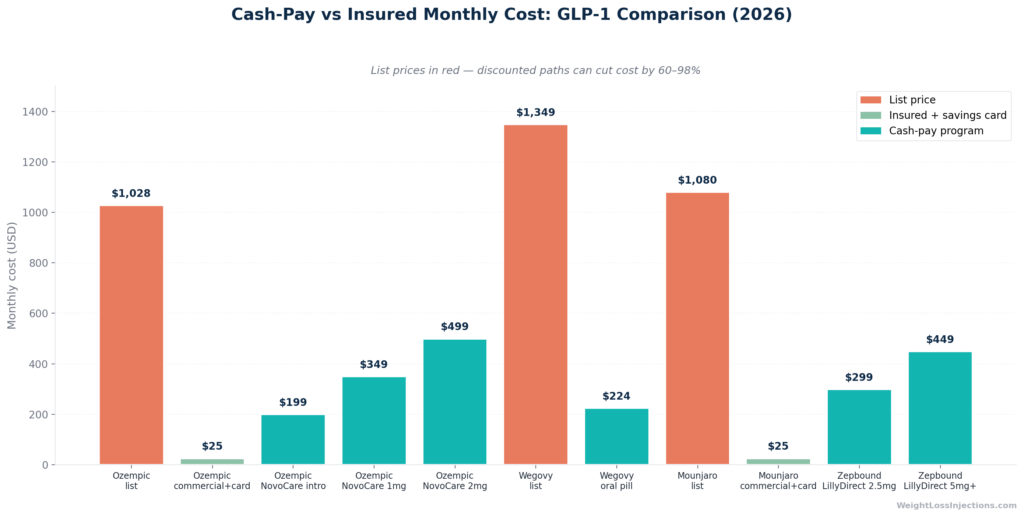
Cash-Pay vs. Insured Monthly Cost Comparison Bar Chart
| Drug | List Price | Best Insured (T2D, savings card) | Best Self-Pay |
|---|---|---|---|
| Ozempic (semaglutide inj.) | $1,028/mo | $25/mo | $199/mo intro; $349/mo ongoing |
| Wegovy (semaglutide weight mgmt) | $1,349/mo | $25/mo | $149–$299/mo (oral pill, NovoCare) |
| Mounjaro (tirzepatide T2D) | ~$1,080/mo | $25/mo | Requires commercial ins. (~$499–$600) |
| Zepbound (tirzepatide weight mgmt) | ~$1,080/mo | $25/mo | $299–$449/mo (LillyDirect vials) |
Sources: Ozempic.com; GoodRx Ozempic; SHARED_SPEC verified facts, April 2026
A few key distinctions worth noting:
- Mounjaro has no self-pay program for the truly uninsured. The savings card requires at least commercial insurance of some kind. Ozempic’s NovoCare program is available to patients with zero insurance.
- Wegovy’s new oral pill (launched January 2026) is available through NovoCare Pharmacy at $149–$299/mo, making it a competitive self-pay option for patients who prefer the labeled weight-loss indication.
- The $675/mo list price reset announced by Novo Nordisk in February 2026 applies to all Ozempic forms starting 2027, not 2026 pricing.
Why Telehealth Cash-Pay Can Beat the Insurance Route
For patients pursuing Ozempic primarily for weight management, where insurance coverage is inconsistent, PA requirements are burdensome, and denials are common, the math on telehealth bundled programs often works out favorably.
The insurance route for off-label weight-loss Ozempic involves: formulary lookup, prescriber PA submission (typically taking two to six weeks for commercial, per IvyRx’s Medicaid analysis), potential step therapy requirements, possible denial and appeal, and then if approved, managing a specialty-pharmacy workflow. Against that backdrop, a bundled telehealth program that includes the consultation, medication, and shipping in one monthly price removes the administrative overhead entirely.
Reputable telehealth programs offering Ozempic or equivalent semaglutide products as part of a supervised weight-management program typically run $300–$500/mo all-in, bundling prescriber visits, dose escalation guidance, and pharmacy dispensing. At WeightLossInjections.com, a supervised weight-loss program starts at [$X/month], including [service detail]. No prior authorization, no step therapy, no appeals process. The trade-off is that costs do not count toward any commercial or Medicare deductible or OOP maximum, which matters only if you expect to reach those thresholds anyway.
Our take at WeightLossInjections.com: If you have commercial insurance actively covering Ozempic for T2D, use it, $25/mo with the savings card is genuinely hard to beat. If you are pursuing Ozempic for weight loss without a T2D diagnosis, or if your plan has denied the claim and your appeal timeline is weeks out, a bundled telehealth program at $300–$500/mo is a more predictable and often faster path than fighting an insurer on off-label coverage.
Frequently Asked Questions
Does Medicare cover Ozempic for weight loss in 2026?
No, not under standard Part D rules. Federal law prohibits Medicare from covering drugs prescribed solely for weight loss, per the Medicare Prescription Drug, Improvement, and Modernization Act. Medicare Part D covers Ozempic for its three FDA-approved indications: type 2 diabetes glycemic control, cardiovascular risk reduction in T2D patients with established CV disease, and CKD risk reduction in T2D patients. A six-month BALANCE Model bridge program is scheduled to launch July 2026, offering GLP-1 weight-management drugs (Wegovy, Zepbound) at $50/mo to qualifying Medicare beneficiaries, but Ozempic is not a labeled weight-loss drug and is not included in that program for the weight-loss indication, per AARP’s February 2026 analysis.
How much is Ozempic with commercial insurance and the savings card?
With commercial insurance that covers Ozempic for type 2 diabetes and the Novo Nordisk savings card activated, eligible patients pay as little as $25/mo for any dose. The maximum plan-covered savings is $100/month (or $200/$300 for 2- or 3-month supplies), valid for up to 48 months from enrollment, per Ozempic.com savings terms. Government beneficiaries, Medicare, Medicaid, TRICARE, VA, do not qualify for the savings card. Without the savings card, specialty-tier copays typically range from $50 to $150/mo depending on the plan’s tier structure.
What is the NovoCare cash price for Ozempic?
Novo Nordisk offers direct self-pay pricing through the NovoCare Pharmacy for uninsured or self-paying patients. New patients pay $199/mo for the first two fills of Ozempic 0.25 mg or 0.5 mg, an introductory offer valid through June 30, 2026. After the introductory period (or for ongoing patients): $349/mo for 0.25 mg, 0.5 mg, or 1 mg; $499/mo for the 2 mg dose. GoodRx coupon pricing mirrors these tiers as of April 2026. Government beneficiaries are excluded from NovoCare self-pay programs.
Can I get Ozempic free through the patient assistance program?
Possibly, if you meet strict eligibility criteria. The NovoCare Patient Assistance Program (PAP) provides Ozempic at no cost to uninsured, low-income patients with a household income at or below 200% of the federal poverty level, a tighter threshold than Novo Nordisk’s PAP for its other products (which allow up to 400% FPL). Patients with commercial insurance, Medicaid, VA benefits, or enrollment in Medicare Low Income Subsidy (Extra Help) are not eligible. Crucially, most Medicare Part D patients are now excluded from Ozempic PAP because Part D covers the drug. If you have Medicare and struggle with costs, the Part D Extra Help / LIS program and the $2,100 OOP cap are the relevant pathways.
Why choose telehealth for Ozempic if insurance denies?
When insurance denies Ozempic, particularly for the weight-loss indication, the appeal process can take weeks, involves prescriber time and documentation burden, and still carries a material denial risk. Telehealth programs that bundle the prescription, clinical oversight, and delivery into a flat monthly fee typically cost $300–$500/mo, compared to the $1,028 list price without any program, or the $349 NovoCare ongoing cash price (medication only, no clinical support). The bundled model is particularly valuable for weight-management patients who need regular dose titration, access to a prescriber for side effect management, and a consistent supply without PA games. WeightLossInjections.com offers supervised GLP-1 programs starting at [$X/month] with [service detail] included, no prior authorization required.
This article is for informational purposes only and does not constitute medical or financial advice. Insurance coverage rules, formulary tiers, savings program terms, and federal policies are subject to change. Verify all pricing and coverage details directly with your insurer, pharmacy, and the manufacturer before making treatment decisions. WeightLossInjections.com’s editorial team reviews content quarterly; last verified April 2026.

